In early 2014, the West African nation of Sierra Leone seemed as though it was finally putting its decade long civil war behind it.
Tens of thousands of people died between 1992-2002 and the recovery was horribly protracted.
Then, in late May 2014, Sierra Leone was faced with another disaster: the Ebola outbreak gripping its neighbours, Guinea and Liberia, had crossed the border.
In the years prior to the outbreak, the country of more than 5.5 million had experienced substantial economic growth.
But the epidemic would have a disastrous effect on the economy, to education and, perhaps worst of all, the country’s healthcare system.
On 7 November 2015 it was announced that the Ebola outbreak had ended in Sierra Leone.
Médecins Sans Frontières/Doctors Without Borders (MSF) first worked in Sierra Leone in 1986.
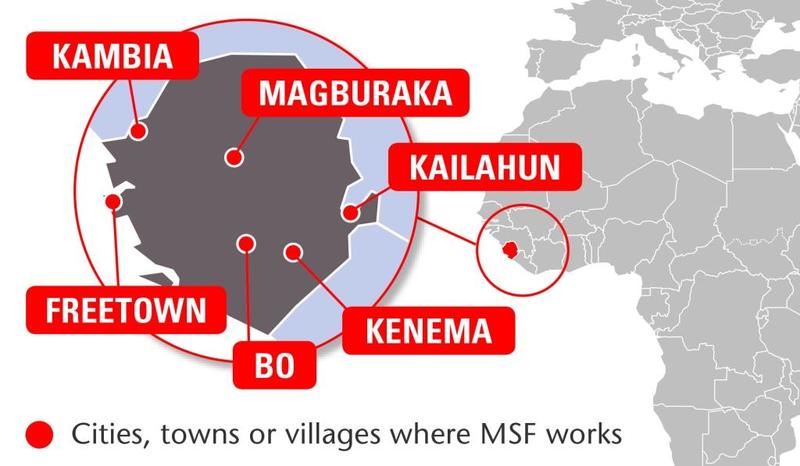
[[Country-Facts]]
MSF’s work in Sierra Leone: 2014
There were new Ebola cases in Sierra Leone during 2015, but the World Health Organization declared the outbreak over on 7 November.
MSF continued its Ebola response, and the 100-bed Prince of Wales School Ebola treatment centre in Freetown provided medical care and psychological support for Ebola patients until February 2015. Of the 400 patients admitted, 170 were confirmed as having the virus. The team performed triage, isolated and tested patients, and ran health promotion activities.
A specialised unit was opened in Freetown in January to care for pregnant women suffering from Ebola, and for their babies, who are particularly vulnerable to the disease.
At the peak of the epidemic, mortality rates for pregnant women reached as high as 90 percent.
Ebola survivor support
Many Ebola survivors are reporting eye and joint problems, as well as anxiety and depression. In February, MSF opened a survivor clinic in Freetown, where the team provided medical and psychological support, referred patients as necessary and ensured free access to ophthalmic care at the Kissy eye hospital.
[[Article-CTA]]
In July, MSF began providing survivor support in Tonkolili district through mobile clinics, and also started running mobile clinics in Kailahun district in December that offered medical consultations and referrals to mobile eye care clinics managed by Partners in Health for specialised care.
Ebola project closures and handovers
The Kailahun treatment centre was closed early in 2015, after Ministry of Health staff received extensive training in biosafety and isolation protocols, the referral process and disease surveillance.
An isolation ward was also built before the handover to manage any cases referred from around the district. The Magburaka treatment centre closed in May and the Bo centre in October.
Tackling measles and malaria
During the Ebola outbreak, routine vaccination schedules fell by the wayside, resulting in a resurgence of preventable diseases. In April, MSF responded to a measles outbreak in Freetown and until June teams supported 10 public health units by training staff, supervising case management and donating medication.
MSF also undertook a mass distribution of antimalarials in Western province in January, reaching over 1.8 million people.
Find out more in our 2015 International Activity Report






