“We left because of the war in Syria, because of fear of this war and the shelling,”
Um Abdullah,[1] a mother of six from Syria’s Dara’a governorate. She closes her eyes and counts off the years on her fingers.
“We came to Jordan almost six years ago. I was afraid for the safety of my children. I had three sons and four daughters, but I lost one of them in the war.”
Buthaina, Um Abdullah’s nine-year-old daughter, sits next to her and gazes at her mother as if hearing these words for the first time.
“There was shelling going on. My son was helping his friends into a basement for shelter. He was standing right by the door when he was injured and died.” Um Abdullah stops to breathe deeply and silence fills the room of the clinic where Doctors Without Borders/Médecins Sans Frontières (MSF) work to treat patients with chronic diseases. She reaches for her coffee and takes a sip, saying with a smile, “Alaa, the MSF nurse here, insists that I take my coffee without sugar, but I was craving one with at least a little sweetness.”
Um Abdullah discovered she had diabetes three years ago when she went for surgery and tests showed a high level of sugar in her blood. She took the news calmly.
“I was preoccupied with the fact that I was about to undergo surgery and was just too busy to think about blood sugar,”

Taking another sip of coffee, Um Abdullah looks at her daughter.
“Buthaina was four years old when the shelling and bombing were happening in Syria,”
“Just a week after we arrived in Jordan, she got stuck in an elevator and it took us an hour to get her out. The next day, her breath smelt bad. And sometimes when she played games, she felt faint and had to stop. We knew we shouldn’t wait any longer, so we took her to the hospital. When her test results came, we learnt that she had type 1 diabetes. Her blood sugar was at 350 and her pancreas had stopped working. She was only four years old. That’s when it all started.”
Her daughter excuses herself to run to the restroom, and Um Abdullah carries on speaking:
“We don’t have diabetes in the family – my daughter’s diabetes is not hereditary. No one believes me, but I think it is psychologically related. Syrians, living with the war – we all became hypertensive and diabetic.”
With an eye on the door for her daughter’s return, she continues:
“When she was seven, Buthaina began experiencing difficulties accepting her disease. She started at school, where she saw her friends eating biscuits and chocolates and drinking Coca Cola. She felt different when she saw that they could choose freely what to eat while she couldn’t.”
Um Abdullah puts her coffee cup down on the nearby table before starting to speak again:
“Her father and I live in constant anxiety. We are anxious whenever Buthaina goes to sleep – twice we almost lost her because her blood sugar dropped while she was sleeping. We only find out if it has dropped when she wakes up: her voice clenches as if she has spasms in her throat. As soon as this happens, we mix sugar with water and apply it to her teeth and gums – only then does she start to regain full consciousness – and then we take her to hospital. This is why I like to give her a small piece of chocolate before she goes to sleep, thinking it would be better if her sugar level rises than drops.”

The door opens and Buthaina comes in. Sitting back down, she listens to the conversation and lightly shakes her mother’s arm, wanting to participate but too timid to make her voice heard.
“Buthaina knows her body very well now,”
“She knows when her sugar level drops and when it is high. She does her diabetes test by herself and compares her readings. I am proud to see her being so responsible.”
How have Um Abdullah and her husband managed to pay for Buthaina’s long-term care?
“At first we visited the hospital and the hospital provided us with insulin,”
“Afterwards, they told us that Syrians were no longer accepted at the hospital and so we started looking for alternatives.”
During their search for healthcare options in the area, they heard about MSF from a neighbour.
“He said that MSF was registering patients, so I hurried to the clinic and the staff immediately registered us,”
“Now we have an appointment scheduled every month. Our medication is expensive but MSF provides it for us free of charge.”
Um Abdullah and Buthaina get ready to leave. At the door, Um Abdullah turns again hesitantly, as if with an urge to say something that has been on her mind since she came in.
“One of the reasons why I haven’t returned to Syria is because of Buthaina’s diabetes,”
“I’m very concerned that she wouldn’t be able to find the kind of healthcare she has here, and it’s difficult to find insulin back home. Even the strips used for the daily diabetes analysis are not available in Syria. Her treatment could easily be interrupted. Imagine a diabetic patient whose insulin dosage is interrupted for one day: that would be it for them.”
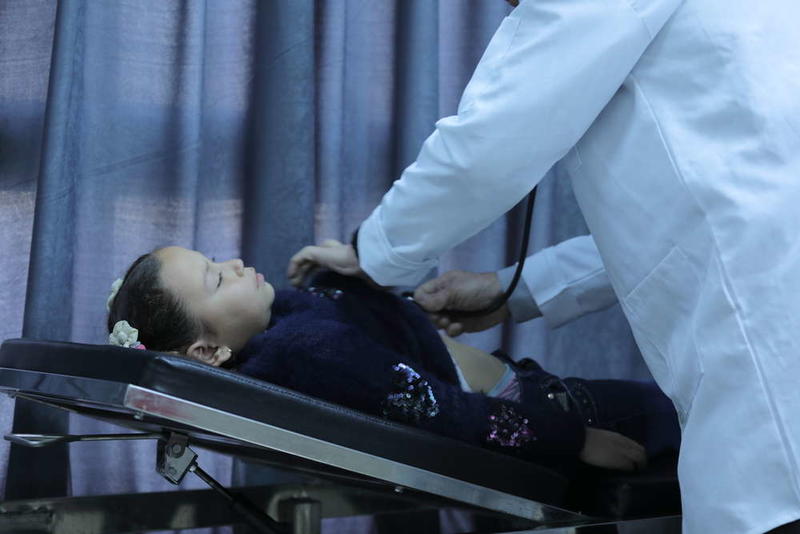
With every mention of Syria, Um Abdullah’s emotions come to the surface, despite her attempts to conceal them.
“If the war stops, I will go back to my country, Syria,”
“After we left, I realised how valuable and precious my homeland is. But most importantly, if I could guarantee good healthcare for my daughter there, I would go back instantly.”
**Names have been changed.
[1] ‘Mother of Abdullah’: Traditionally, fathers and mothers in the Middle East are referred to by their eldest son’s name.
In December 2014, MSF opened a non-communicable diseases (NCDs) project in Irbid governorate with two clinics, providing medical treatment for Syrian refugees and vulnerable Jordanians with a range of chronic diseases, including diabetes, hypertension, asthma, cardiovascular diseases and chronic obstructive pulmonary disease. In August 2015, MSF launched its home visit programme to reach patients who could not visit the clinics because of physical disability or financial constraints. The NCD project also provides health education and psychosocial support to help patients lead healthy lives.
At present, MSF has 3,374 patients enrolled in its NCDs project in Irbid; 2,113 (62.6%) of them are being treated for both types of diabetes. MSF teams have provided 58,181 consultations, including home visits, since the start of the NCDs project in December 2014.





