Um Yousef[1] is a Jordanian teacher at a government school.
“Mustafa has been suffering from diabetes for four years now. It all happened over 10 days.”
“I noticed that my son was losing weight and was going to the restroom a lot, and so I said that I would take him to the doctor on the Saturday, as that’s my day off.”
“In the meantime, we were invited to my nephew’s engagement party, where my son ate kunafa[2] and drank juice. That night, he didn’t feel well at all – he was running a high fever and was hallucinating. I took him to the clinic and the doctor asked the nurses to do some tests. When the results came out, the doctor was hesitant about telling me the results – he thought I looked so worried that my husband should be with me.”
The results showed that Mustafa’s blood sugar level stood at 467 and his triglycerides were high, indicating that he had diabetes.
Um Yousef was astonished at the results.
“How could he have diabetes at this young age?”
The doctor explained that more than 50 percent of cases of juvenile diabetes are not hereditary, but happen suddenly after the pancreas malfunctions and produces little or no insulin.
Um Yousef was devastated at the diagnosis.
“I always saw him as a healthy, active young boy,”
“He was too young to live with this disease – he was only eight when he was diagnosed with diabetes.”
Four years later, Mustafa is undergoing regular medical treatment provided by Doctors Without Borders/Médecins Sans Frontières (MSF) at a clinic in Jordan’s Irbid governorate, and his mother has come to terms with his condition.
“I leave work in the afternoon at the same time as Mustafa’s medication time,”
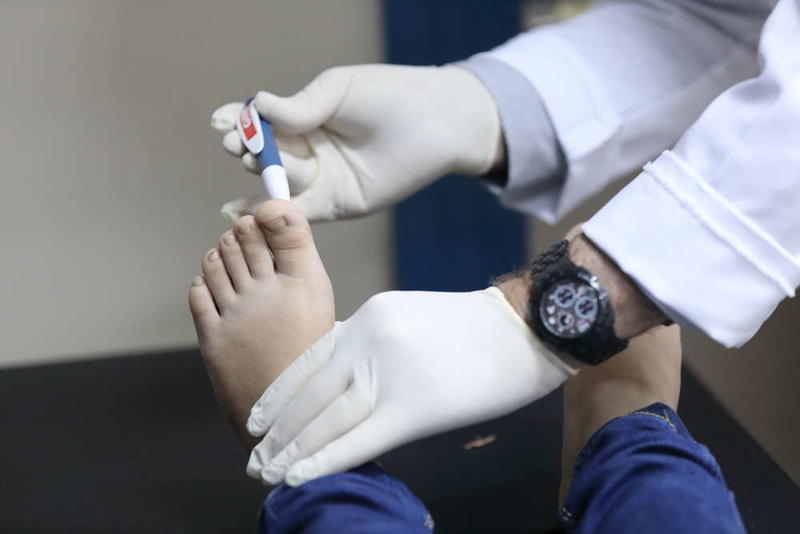
“So he does his sugar blood test by himself and, depending on the reading, I give him the dose of insulin.”
However, Mustafa’s blood sugar readings are still higher than they should be, according to the doctors and nurses at MSF’s clinic.
“Mustafa still isn’t committed to following medical orders, and it seems that he hasn’t fully accepted the disease,”
“The mental health counsellor in the clinic is working hard with him so that he will accept it eventually.”
A small note of defeat can be sensed in Um Yousef’s tone.
To help Mustafa, the entire family worked together to make his condition seem normal.
“We introduced brown bread and sugar-free biscuits,”
“But he wouldn’t eat them. He kept asking me difficult questions like, ‘Why are my brothers eating whatever they want while I’m not allowed to?’”

They realised that having one diabetic in the family affected them all.
“You can’t see your child discontented and deprived of the pleasures he once had and be content yourself,”
“We had to help him adapt, so we deprived ourselves, including his brothers, of certain things which we liked but which we knew could harm Mustafa’s health. But still, he’d find ways to buy the things he wanted, especially during school hours when there was no one to watch over him.”
MSF’s doctor now sees Mustafa every two weeks to monitor his blood sugar levels closely. But something different has happened this time: his blood sugar reading has gone down. The doctor says it shows an improvement and more control over the disease. Um Yousef turns to her son looking happy and Mustafa smiles back at her, delighted with his accomplishment and feeling triumphant at last.
** Names have been changed.
[1] Mother of Yousef: Traditionally, fathers and mothers in the Middle East are referred to by their eldest son’s name.
[2] A very sweet Levantine dessert.

In December 2014, MSF opened a non-communicable diseases (NCDs) project in Irbid governorate with two clinics, providing medical treatment for Syrian refugees and vulnerable Jordanians with a range of chronic diseases, including diabetes, hypertension, asthma, cardiovascular diseases and chronic obstructive pulmonary disease. In August 2015, MSF launched its home visit programme to reach patients who could not visit the clinics because of physical disability or financial constraints. The NCD project also provides health education and psychosocial support to help patients lead healthy lives.
At present, MSF has 3,374 patients enrolled in its NCDs project in Irbid; 2,113 (62.6%) of them are being treated for both types of diabetes. MSF teams have provided 58,181 consultations, including home visits, since the start of the NCDs project in December 2014.





